CIDPUSA.ORG ❤
Autoimmune Diseases Web Search Page
Search CIDPUSA WEBSITE Alternative Treatments
Special Google Health SearchCIDPUSA.org
Information MyatheniaCIDPUSA Foundation alternatives treatment of autoimmune disease read our e-book
Natural Myasthenia courseGirl with Myasthenia ptosis in both eyes
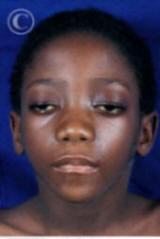 Eye
Lids Drooping in Myasthenia
Today all forms of myasthenia are treatable!
Eye
Lids Drooping in Myasthenia
Today all forms of myasthenia are treatable!Myasthenia is caused by autoimmune process
. Learn to turn off inflammation at the source. What is myasthenia gravis?Myasthenia gravis is a chronic autoimmune neuromuscular disease characterized by varying degrees of weakness of the muscles of the body. The name myasthenia gravis, literally means "grave muscle weakness." With current therapies, however, most cases of myasthenia gravis are not as "grave" as the name implies. In fact, for the majority of individuals with myasthenia gravis, life expectancy is not lessened by the disorder.
The hallmark of myasthenia gravis is muscle weakness that increases during periods of activity and improves after periods of rest. Certain muscles such as those that control eye and eyelid movement, facial expression, chewing, talking, and swallowing are often, but not always, involved in the disorder. The muscles that control breathing and neck and limb movements may also be affected.
In myasthenia gravis, antibodies block, alter, or destroy the receptors for acetylcholine at the neuromuscular junction which prevents the muscle contraction from occurring. These antibodies are produced by the body's own immune system. Thus, myasthenia gravis is an autoimmune disease because the immune system - which normally protects the body from foreign organisms - mistakenly attacks itself.
The normal neuromuscular junction is affected in myasthenia gravis. The antibodies bind to the acetylcholine (Ach) receptor preventing binding of the neurotransmitter (Ach).
What is the role of the thymus gland in myasthenia gravis?
The thymus gland, which lies in the upper chest area beneath the breastbone, plays an important role in the development of the immune system in early life. Its cells form a part of the body's normal immune system. The gland is somewhat large in infants, grows gradually until puberty, and then gets smaller and is replaced by fat with age. In adults with myasthenia gravis, the thymus gland is abnormal. It contains certain clusters of immune cells indicative of lymphoid hyperplasia - a condition usually found only in the spleen and lymph nodes during an active immune response. Some individuals with myasthenia gravis develop thymomas or tumors of the thymus gland.
The relationship between the thymus gland and myasthenia gravis is not yet fully understood.
What are the symptoms of myasthenia gravis?
Although myasthenia gravis may affect any voluntary muscle, muscles that control eye and eyelid movement, facial expression, and swallowing are most frequently affected. The onset of the disorder may be sudden. Symptoms often are not immediately recognized as myasthenia gravis.
In most cases, the first noticeable symptom is weakness of the eye muscles. In others, difficulty in swallowing and slurred speech may be the first signs. The degree of muscle weakness involved in myasthenia gravis varies greatly among patients, ranging from a localized form, limited to eye muscles (ocular myasthenia), to a severe or generalized form in which many muscles - sometimes including those that control breathing - are affected. Symptoms, which vary in type and severity, may include a drooping of one or both eyelids (ptosis), blurred or double vision (diplopia) due to weakness of the muscles that control eye movements, unstable or waddling gait, weakness in arms, hands, fingers, legs, and neck, a change in facial expression, difficulty in swallowing and shortness of breath, and impaired speech (dysarthria).
topWho gets myasthenia gravis?
Myasthenia gravis occurs in all ethnic groups and both genders. It most commonly affects young adult women (under 40) and older men (over 60), but it can occur at any age and many are vitamin-D deficient this alone may improve the person.
In neonatal myasthenia, the fetus may acquire immune proteins (antibodies) from a mother affected with myasthenia gravis. Generally, cases of neonatal myasthenia gravis are transient (temporary) and the child's symptoms usually disappear within 2-3 months after birth. Other children develop myasthenia gravis indistinguishable from adults. Myasthenia gravis in juveniles is common.
Myasthenia gravis is not directly inherited nor is it contagious. Occasionally, the disease may occur in more than one member of the same family.
Rarely, children may show signs of congenital myasthenia or congenital myasthenic syndrome. These are not autoimmune disorders, but are caused by defective genes that produce proteins in the acetylcholine receptor or in acetylcholinesterase.
How is myasthenia gravis diagnosed?
The first steps of diagnosing myasthenia gravis include a review of the individual's medical history, and physical and neurological examinations. The signs a physician must look for are impairment of eye movements or muscle weakness without any changes in the individual's ability to feel things. If the doctor suspects myasthenia gravis, several tests are available to confirm the diagnosis.
A special blood test can detect the presence of immune molecules or acetylcholine receptor antibodies. Most patients with myasthenia gravis have abnormally elevated levels of these antibodies. However, antibodies may not be detected in patients with only ocular forms of the disease.
Another test is called the edrophonium test. This approach requires the intravenous administration of edrophonium chloride or Tensilon(r), a drug that blocks the degradation (breakdown) of acetylcholine and temporarily increases the levels of acetylcholine at the neuromuscular junction. In people with myasthenia gravis involving the eye muscles, edrophonium chloride will briefly relieve weakness.
A different test called single fiber electromyography (EMG), in which single muscle fibers are stimulated by electrical impulses, can also detect impaired nerve-to-muscle transmission. EMG measures the electrical potential of muscle cells. Muscle fibers in myasthenia gravis, as well as other neuromuscular disorders, do not respond as well to repeated electrical stimulation compared to muscles from normal individuals. Computed tomography (CT) may be used to identify an abnormal thymus gland or the presence of a thymoma.
A special examination called pulmonary function testing - which measures breathing strength - helps to predict whether respiration may fail and lead to a myasthenic crisis.
How is myasthenia gravis treated?
Thymectomy, the surgical removal of the thymus gland (which often is abnormal in myasthenia gravis patients), reduces symptoms in more than 70 percent of patients without thymoma and may cure some individuals, possibly by re-balancing the immune system. Other therapies used to treat myasthenia gravis include plasmapheresis, a procedure in which abnormal antibodies are removed from the blood, and high-dose intravenous immune globulin,
What are myasthenic crises?
What is the prognosis?
With treatment, the outlook for most patients with myasthenia gravis is they can expect to lead normal or nearly normal lives. Some cases of myasthenia gravis may go into remission temporarily and muscle weakness may disappear completely so that medications can be discontinued. . Toxins in our body blocks our proper body functions, shuts down the immune system and causes a long list of chronic diseases.Vitamin D & intravenous immune globulin, makes a differnce !
continued to cidp-studies page